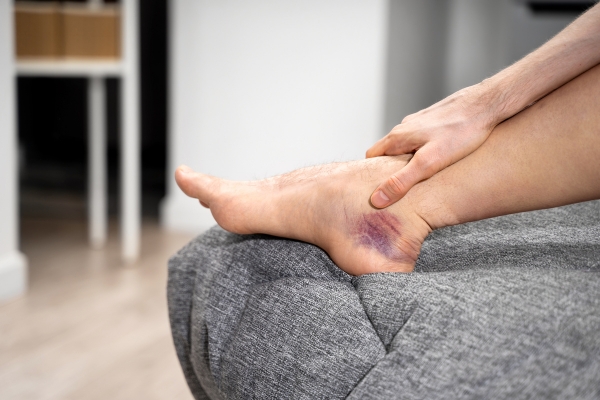
Venous stasis ulcers are one of the most serious complications of untreated venous disease, and more common than patients may realize. These open wounds can take weeks or months to close and can progress to infections and permanent tissue damage without proper care.
Due to these risks, it’s important to let your doctor know about concerning symptoms and practice lifestyle habits that support blood flow.
What Are Venous Ulcers and How Do They Develop?
Venous stasis ulcers occur when changes in circulation limit blood flow throughout the body. For patients with chronic venous insufficiency, varicose veins, or venous reflux disease, damage to the vein valves can lead to fluid accumulation and pressure on the skin and muscle tissue. Leaving this issue unaddressed may lead to ulcers on the lower legs or around the ankles.
The small size of venous stasis ulcers may make it easy to dismiss them as a cut or scrape. Patients may also experience symptoms such as leg pain, itching, swelling, changes in skin color or texture and foul-smelling discharge.
Risks for venous ulcers increase in patients with:
- A Venous Disorder: This includes conditions like varicose veins, chronic venous insufficiency, a venous obstruction, venous reflux, high blood pressure, thrombosis and phlebitis.
- Certain Lifestyle Habits: Carrying excess weight and a history of smoking can restrict circulation and damage the valves responsible for circulating oxygen-rich blood.
- Other Medical Conditions: Diabetes or paralysis increase ulcer risks due to nerve damage, dry skin and impaired healing response.
How Can You Prevent Venous Ulcers?
Following a daily routine that promotes healthy circulation helps lower your risk of venous stasis ulcers.
- Elevate Your Legs: Raising your legs above your heart for 10 to 20 minutes a day supports proper blood circulation and helps reduce pressure in the lower extremities.
- Do Leg Exercises: Stronger leg muscles help deep veins push blood up towards the heart.
- Wear Compression Stockings: These therapeutic stockings work to enhance circulation in the legs, helping reduce risk factors for venous ulcers, such as fluid pooling and swelling.
- Maintain Healthy Weight: Losing a few extra pounds can reduce strain on your circulatory system, helping to improve blood flow throughout the body.
- Quit Smoking: Smokers have a higher risk of blood clots, ulcers, stroke, heart attack and peripheral artery disease due to the impact of this habit on the blood vessels.
How to Manage Venous Stasis Ulcers
If not properly treated, venous ulcers can cause permanent tissue damage and life-threatening infections. It’s important to consult with an experienced medical provider to determine the best way to address them.
Management starts with addressing the underlying issue and caring for ulcer-prone skin appropriately.
- Hydration: Applying barrier cream can improve skin hydration and moisture retention while lowering the risks of fissures and delayed wound healing.
- Debridement: Cleaning and removing dead tissue from the wound helps the healing process while managing infection concerns.
- Compression Therapy: This treatment keeps blood moving back to the heart, relieving the pressure on your leg veins and helping ulcers heal sooner.
- Antibiotics: Patients may be given an oral or topical antibiotic to control infection risks that could impair healing or lead to more serious complications.
Do You Have Untreated Varicose Veins?
If you’re living with varicose veins, chronic venous insufficiency or a wound that isn’t healing, our specialists at Vein Centers of Connecticut can assess your risk and develop a treatment plan before serious complications develop. Schedule a consultation today.
